What Is Pudendal Neuralgia?
Pudendal neuralgia is a condition characterized by chronic pain in the pelvic region, specifically affecting the pudendal nerve, which is responsible for sensation and function in the genital area, perineum, and anus. This nerve can become compressed or irritated, leading to a range of uncomfortable symptoms that can significantly impact a person’s quality of life.
The pudendal nerve originates from the sacral plexus, which is a network of nerves in the lower back. It travels through the pelvis and innervates various structures, including the external genitalia and the anal sphincter. When this nerve is compromised, it can result in debilitating pain and discomfort.
Causes of Pudendal Neuralgia
Understanding the causes of pudendal neuralgia is crucial for effective management. Some common causes include:
- Trauma or Injury: Direct trauma to the pelvic area, such as from childbirth or surgery, can lead to nerve damage.
- Prolonged Sitting: Activities that involve long periods of sitting, such as cycling or sitting on hard surfaces, can compress the pudendal nerve.
- Pelvic Floor Dysfunction: Conditions affecting the pelvic floor muscles can contribute to nerve irritation.
- Infections: Certain infections in the pelvic region may also irritate the pudendal nerve.
Identifying the underlying cause is essential for developing an effective treatment plan. If you suspect you may be experiencing symptoms of pudendal neuralgia, consulting a healthcare professional is vital.
Pudendal Neuralgia Symptoms
The symptoms of pudendal neuralgia can vary widely among individuals, but they typically include:
Common Symptoms
- Chronic Pain: This is the hallmark symptom, often described as sharp, burning, or aching pain in the pelvic region.
- Genital Discomfort: Many individuals report discomfort in the genital area, which can be exacerbated by sitting or sexual activity.
- Perineal Pain: Pain may also radiate to the perineum, the area between the genitals and the anus.
- Urinary Issues: Some may experience urinary urgency, frequency, or incontinence.
- Changes in Sexual Function: Pudendal neuralgia can lead to difficulties with arousal, orgasm, or pain during intercourse.
Symptoms in Men vs. Women
While pudendal neuralgia can affect anyone, there are some differences in how symptoms may present in men and women:
- Men: In men, symptoms may include pain in the scrotum or penis, and issues related to erectile dysfunction.
- Women: Women may experience more pronounced symptoms related to the vulva and vagina, including pain during intercourse and increased sensitivity.
It’s important to note that symptoms can fluctuate, with some individuals experiencing periods of relief followed by flare-ups. Keeping a symptom diary can help identify triggers and patterns, which can be beneficial for treatment discussions with healthcare providers.
When to Seek Help
If you are experiencing persistent pelvic pain or any of the symptoms mentioned above, it is crucial to seek medical advice. Early diagnosis and intervention can lead to better outcomes and improved quality of life. Healthcare professionals may recommend a variety of treatment options, including physical therapy, medications, or even nerve blocks, depending on the severity and underlying causes of the condition.
For more information and resources on managing pudendal neuralgia, consider visiting Yesil Health AI, where you can find evidence-based answers to your health questions.
In conclusion, pudendal neuralgia is a complex condition that requires a comprehensive approach to diagnosis and treatment. Understanding the symptoms and seeking timely help can make a significant difference in managing this challenging condition. 🌟
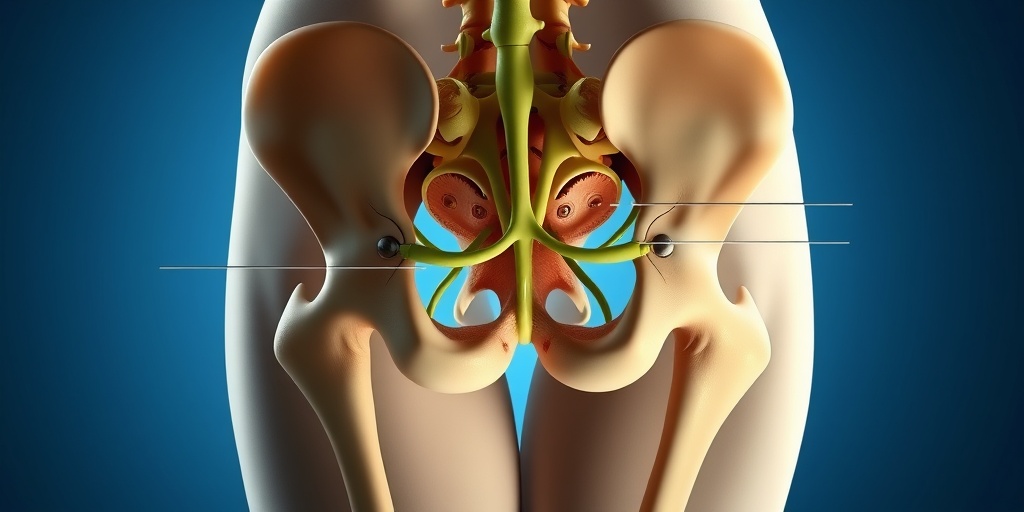
Pudendal Neuralgia Causes
Pudendal neuralgia is a condition characterized by chronic pain in the pelvic region, often affecting the genital area, perineum, and buttocks. Understanding the causes of pudendal neuralgia is crucial for effective management and treatment. Here are some of the primary causes associated with this condition:
1. Nerve Compression
One of the most common causes of pudendal neuralgia is compression of the pudendal nerve. This can occur due to:
- Prolonged sitting: Sitting for extended periods, especially on hard surfaces, can put pressure on the pudendal nerve.
- Injury: Trauma to the pelvic area, such as from accidents or surgical procedures, can lead to nerve damage or compression.
- Childbirth: The physical stress of childbirth can sometimes result in nerve compression or injury.
2. Pelvic Floor Dysfunction
Pelvic floor dysfunction can also contribute to pudendal neuralgia. This condition occurs when the muscles of the pelvic floor become weak or overly tight, leading to:
- Muscle spasms: Tight pelvic floor muscles can irritate the pudendal nerve.
- Increased pressure: Dysfunction in the pelvic floor can create additional pressure on the nerve, exacerbating pain.
3. Infections and Inflammation
Infections in the pelvic region, such as prostatitis in men or vulvodynia in women, can lead to inflammation that affects the pudendal nerve. Conditions like pelvic inflammatory disease (PID) can also contribute to nerve irritation.
4. Structural Abnormalities
Certain anatomical issues can predispose individuals to pudendal neuralgia. These may include:
- Pelvic tumors: Growths in the pelvic area can exert pressure on the pudendal nerve.
- Spinal issues: Problems in the lower spine, such as herniated discs, can lead to nerve compression.
5. Other Medical Conditions
Several medical conditions can increase the risk of developing pudendal neuralgia, including:
- Diabetes: This condition can lead to nerve damage over time, increasing the risk of pudendal neuralgia.
- Multiple sclerosis: Neurological disorders can affect nerve function and lead to pain syndromes.
Pudendal Neuralgia Risk Factors
Identifying the risk factors for pudendal neuralgia can help in early diagnosis and prevention. Here are some key factors that may increase the likelihood of developing this condition:
1. Gender
Research indicates that pudendal neuralgia is more prevalent in women than in men. This may be attributed to anatomical differences and the impact of childbirth on the pelvic region.
2. Age
Age can also play a significant role in the development of pudendal neuralgia. Older adults may experience a higher incidence due to age-related changes in nerve function and pelvic floor integrity.
3. Lifestyle Factors
Certain lifestyle choices can increase the risk of pudendal neuralgia:
- Prolonged sitting: Occupations or activities that require long periods of sitting can contribute to nerve compression.
- Obesity: Excess weight can put additional pressure on the pelvic area, increasing the risk of nerve irritation.
4. Physical Activity
While regular exercise is beneficial, certain high-impact activities or sports that involve repetitive pelvic movements may increase the risk of pudendal nerve injury. Activities such as cycling or horseback riding can be particularly problematic.
5. Previous Pelvic Surgery
Individuals who have undergone pelvic surgery may be at a higher risk for pudendal neuralgia due to potential nerve damage or scarring that can occur during surgical procedures.
Understanding the causes and risk factors associated with pudendal neuralgia is essential for those experiencing symptoms. If you suspect you may have this condition, consulting a healthcare professional for a thorough evaluation and personalized treatment plan is crucial. 🩺

Pudendal Neuralgia Diagnosis
Pudendal neuralgia is a condition that can significantly impact a person’s quality of life, often causing discomfort and pain in the pelvic region. Diagnosing this condition can be challenging due to its complex nature and the overlap of symptoms with other pelvic disorders. Here, we’ll explore the diagnostic process for pudendal neuralgia, including the symptoms to watch for and the tests that may be conducted.
Recognizing the Symptoms
The first step in diagnosing pudendal neuralgia is recognizing its symptoms. Common symptoms include:
- Pelvic pain: This can be sharp, burning, or aching and may worsen with sitting.
- Genital discomfort: Patients often report pain in the vulva or perineum.
- Urinary issues: This may include urgency, frequency, or pain during urination.
- Sexual dysfunction: Pain during intercourse is a common complaint.
- Radiating pain: Pain may radiate to the buttocks, thighs, or lower back.
If you experience any of these symptoms, it’s essential to consult a healthcare professional for a thorough evaluation. 🩺
Medical History and Physical Examination
During your visit, your doctor will take a detailed medical history, asking about your symptoms, their duration, and any previous treatments. A physical examination will often focus on the pelvic area to assess tenderness and pain response. This examination may include:
- Neurological assessment: To check for any nerve-related issues.
- Pelvic examination: To evaluate for any abnormalities or sources of pain.
Diagnostic Tests
While there is no single test for pudendal neuralgia, several diagnostic tests can help rule out other conditions and confirm the diagnosis:
- Imaging studies: MRI or CT scans may be used to visualize the pelvic region and identify any structural issues.
- Nerve conduction studies: These tests measure the electrical activity of the pudendal nerve.
- Pelvic floor assessment: This may involve specialized tests to evaluate muscle function and nerve response.
In some cases, a pudendal nerve block may be performed, where a local anesthetic is injected to see if it alleviates pain, confirming the diagnosis. 🧪
Pudendal Neuralgia Treatment Options
Once diagnosed, managing pudendal neuralgia involves a multifaceted approach tailored to the individual’s symptoms and needs. Treatment options can range from conservative measures to more invasive procedures. Here’s a breakdown of the most common treatment strategies.
Conservative Treatments
Many patients find relief through conservative treatments, which may include:
- Physical therapy: Specialized pelvic floor physical therapy can help strengthen muscles and alleviate pain.
- Medications: Pain relievers, anti-inflammatory drugs, and medications for nerve pain (like gabapentin) may be prescribed.
- Heat and cold therapy: Applying heat or ice packs can help reduce inflammation and pain.
- Dietary changes: Some patients find that certain foods exacerbate their symptoms, so keeping a food diary may help identify triggers.
Interventional Treatments
If conservative measures are ineffective, your doctor may recommend interventional treatments, such as:
- Pudendal nerve blocks: As mentioned earlier, these can provide temporary relief and help confirm the diagnosis.
- Botox injections: These can help relax the pelvic floor muscles and reduce pain.
- Radiofrequency ablation: This procedure uses heat to disrupt nerve function and alleviate pain.
Surgical Options
In rare cases where other treatments have failed, surgical options may be considered. These can include:
- Pudendal nerve decompression: This surgery aims to relieve pressure on the pudendal nerve.
- Pelvic floor reconstruction: If structural issues are contributing to the pain, surgical correction may be necessary.
It’s crucial to discuss all treatment options with your healthcare provider to determine the best course of action for your specific situation. Remember, managing pudendal neuralgia often requires a combination of therapies tailored to your unique needs. 🌟

Pudendal Neuralgia Management Strategies
Pudendal neuralgia is a condition that can significantly impact a person’s quality of life, causing chronic pain in the pelvic region. Managing this condition effectively requires a multifaceted approach. Here are some strategies that can help alleviate symptoms and improve overall well-being.
Understanding the Condition
Before diving into management strategies, it’s essential to understand what pudendal neuralgia is. This condition arises from irritation or damage to the pudendal nerve, which supplies sensation to the genital area, perineum, and anus. Symptoms can include:
- Chronic pelvic pain
- Burning or stabbing sensations
- Discomfort during sitting
- Sexual dysfunction
Physical Therapy
One of the most effective management strategies for pudendal neuralgia is physical therapy. A specialized pelvic floor physical therapist can help:
- Strengthen pelvic floor muscles
- Improve flexibility and range of motion
- Teach relaxation techniques to reduce muscle tension
Exercises may include stretching, strengthening, and breathing techniques that focus on the pelvic area. Regular sessions can lead to significant improvements in pain levels and functionality. 🧘♀️
Medication Management
Medications can play a crucial role in managing pudendal neuralgia. Common options include:
- Antidepressants: These can help alleviate chronic pain.
- Anticonvulsants: Medications like gabapentin can reduce nerve pain.
- Topical treatments: Creams or patches containing lidocaine may provide localized relief.
It’s essential to consult with a healthcare provider to determine the best medication regimen tailored to individual needs. 💊
Alternative Therapies
In addition to traditional treatments, several alternative therapies may offer relief:
- Acupuncture: This ancient practice may help reduce pain and improve nerve function.
- Chiropractic care: Adjustments may relieve pressure on the pudendal nerve.
- Massage therapy: Targeted massage can help alleviate muscle tension in the pelvic area.
While these therapies can be beneficial, it’s crucial to work with qualified practitioners who understand pudendal neuralgia. 🌿
Ergonomic Adjustments
For many individuals, sitting can exacerbate symptoms of pudendal neuralgia. Making ergonomic adjustments can help:
- Use a pudendal neuralgia cushion or a specially designed seat to relieve pressure.
- Adjust seating positions to minimize discomfort.
- Take regular breaks to stand and stretch.
These small changes can make a significant difference in daily comfort levels. 🪑
Mind-Body Techniques
Managing chronic pain often requires addressing the psychological aspects as well. Techniques such as:
- Meditation
- Yoga
- Cognitive Behavioral Therapy (CBT)
can help individuals cope with the emotional toll of living with pudendal neuralgia. These practices promote relaxation and can reduce the perception of pain. 🧘♂️
Pudendal Neuralgia Outlook and Prognosis
The outlook for individuals with pudendal neuralgia can vary widely based on several factors, including the underlying cause, the duration of symptoms, and the effectiveness of treatment strategies. Understanding the prognosis can help individuals manage their expectations and plan for the future.
Factors Influencing Prognosis
Several factors can influence the prognosis of pudendal neuralgia:
- Duration of Symptoms: Early intervention often leads to better outcomes.
- Underlying Causes: Conditions such as pelvic trauma or surgery may complicate recovery.
- Response to Treatment: Individuals who respond well to initial treatments often have a more favorable outlook.
Long-Term Management
While some individuals may experience significant relief from symptoms, others may find that pudendal neuralgia is a chronic condition requiring ongoing management. Regular follow-ups with healthcare providers can help:
- Adjust treatment plans as needed
- Monitor for any new symptoms
- Provide support and resources for coping strategies
Staying proactive in managing the condition can lead to improved quality of life. 🌈
Living with Pudendal Neuralgia
Living with pudendal neuralgia can be challenging, but many individuals find ways to adapt and thrive. Support groups, whether online or in-person, can provide a sense of community and shared experiences. Engaging with others who understand the condition can be incredibly beneficial. 💬
In conclusion, while pudendal neuralgia can be a complex and often misunderstood condition, effective management strategies and a positive outlook can significantly enhance the quality of life for those affected. By taking a comprehensive approach to treatment and support, individuals can navigate their journey with greater confidence and resilience.

Frequently Asked Questions about Pudendal Neuralgia
What is Pudendal Neuralgia?
Pudendal Neuralgia is a condition characterized by chronic pain in the pelvic region, often caused by irritation or damage to the pudendal nerve. This nerve is responsible for sensation in the genital area and plays a role in bladder and bowel control.
What are the common symptoms of Pudendal Neuralgia?
- Pelvic pain: Often described as sharp, burning, or aching.
- Discomfort during sitting: Many individuals find it painful to sit for extended periods.
- Sexual dysfunction: This can include pain during intercourse or loss of sensation.
- Urinary issues: Such as urgency or incontinence.
What causes Pudendal Neuralgia?
There are several potential causes of Pudendal Neuralgia, including:
- Trauma: Injury to the pelvic area can lead to nerve damage.
- Prolonged sitting: Activities that involve long periods of sitting can irritate the nerve.
- Childbirth: The pressure during delivery can affect the pudendal nerve.
- Medical conditions: Such as diabetes or multiple sclerosis.
How is Pudendal Neuralgia diagnosed?
Diagnosis typically involves a thorough medical history, physical examination, and may include imaging studies or nerve conduction tests to rule out other conditions.
What are the treatment options for Pudendal Neuralgia?
Treatment for Pudendal Neuralgia may include:
- Physical therapy: Specific exercises can help relieve pressure on the nerve.
- Medications: Pain relievers, anti-inflammatory drugs, or nerve pain medications.
- Injections: Corticosteroid injections may reduce inflammation around the nerve.
- Surgery: In severe cases, surgical intervention may be necessary to relieve nerve compression.
Are there exercises that can help with Pudendal Neuralgia?
Yes, certain exercises can help alleviate symptoms. Pudendal Neuralgia exercises often focus on pelvic floor strengthening and relaxation techniques. Consulting with a physical therapist who specializes in pelvic health is recommended for personalized guidance.
Can men experience Pudendal Neuralgia?
Absolutely! While Pudendal Neuralgia is often discussed in the context of female patients, men can also experience this condition and may have similar symptoms, including pelvic pain and sexual dysfunction.
What is the ICD-10 code for Pudendal Neuralgia?
The ICD-10 code for Pudendal Neuralgia is G57.4, which falls under the category of other mononeuropathies of the lower limb.
Is there a specific cushion recommended for Pudendal Neuralgia?
Yes, many individuals find relief using a pudendal neuralgia cushion, which is designed to reduce pressure on the pelvic area while sitting. These cushions often have a cut-out section to alleviate discomfort.
Where can I find support for Pudendal Neuralgia?
Online communities, such as forums and social media groups, can provide valuable support and shared experiences. Websites like Reddit often have discussions on Pudendal Neuralgia where individuals share their journeys and coping strategies.