What Is Diabetic Nephropathy?
Diabetic nephropathy, often referred to as diabetic kidney disease, is a serious complication that arises from diabetes mellitus. It is characterized by damage to the kidneys due to prolonged high blood sugar levels, which can lead to kidney failure if not managed properly. This condition is one of the leading causes of end-stage renal disease (ESRD) and can significantly impact a person’s quality of life.
The Pathophysiology of Diabetic Nephropathy
The pathophysiology of diabetic nephropathy involves a complex interplay of metabolic and hemodynamic factors. Over time, high glucose levels in the blood can lead to:
- Glomerular Hyperfiltration: Initially, the kidneys may filter blood more efficiently, but this increased workload can cause damage.
- Glomerulosclerosis: The filtering units of the kidneys, known as glomeruli, become scarred and less effective.
- Proteinuria: As the kidneys become damaged, they may allow proteins to leak into the urine, which is a key indicator of nephropathy.
Understanding these mechanisms is crucial for early diagnosis and intervention. If you want to dive deeper into the pathophysiology of diabetic nephropathy, resources like Yesil Health AI can provide evidence-based insights.
Stages of Diabetic Nephropathy
Diabetic nephropathy progresses through several stages, each with distinct characteristics:
- Stage 1: Normal kidney function with increased kidney size and hyperfiltration.
- Stage 2: Mild kidney damage with the presence of microalbuminuria (small amounts of protein in the urine).
- Stage 3: Moderate kidney damage with increased proteinuria and a decline in kidney function.
- Stage 4: Severe kidney damage with significant loss of function, often leading to symptoms of kidney failure.
- Stage 5: End-stage renal disease, requiring dialysis or kidney transplantation.
Recognizing these stages early can help in managing the disease effectively and preventing progression.
Symptoms of Diabetic Nephropathy
Identifying the symptoms of diabetic nephropathy is crucial for timely intervention. Unfortunately, many individuals may not experience noticeable symptoms in the early stages. However, as the disease progresses, several signs may become apparent.
Early Symptoms
In the initial stages, symptoms may be subtle or absent. However, some early indicators include:
- Increased Thirst: A common symptom of diabetes, excessive thirst can also indicate kidney issues.
- Frequent Urination: As kidney function declines, the body may attempt to eliminate excess waste through increased urination.
Advanced Symptoms
As diabetic nephropathy progresses, more pronounced symptoms may develop, including:
- Swelling: Fluid retention can lead to swelling in the legs, ankles, and feet.
- Fatigue: A decline in kidney function can cause a buildup of toxins in the body, leading to fatigue.
- Changes in Urine Color: Dark or foamy urine may indicate the presence of protein.
- High Blood Pressure: Kidney damage can contribute to hypertension, which further exacerbates kidney issues.
Recognizing these symptoms early can lead to better management and treatment options. If you suspect you may be experiencing symptoms of diabetic nephropathy, it’s essential to consult a healthcare professional for a thorough evaluation.
In conclusion, understanding diabetic nephropathy is vital for anyone living with diabetes. By being aware of the symptoms and stages of this condition, individuals can take proactive steps to manage their health effectively. For more information and resources, consider visiting Yesil Health AI, where you can find evidence-based answers to your health questions. 🌟

Causes and Risk Factors
Diabetic nephropathy is a serious complication of diabetes that affects the kidneys, leading to kidney damage and potentially kidney failure. Understanding the causes and risk factors associated with this condition is crucial for prevention and management. Here’s a closer look at what contributes to the development of nephropathy diabetic.
1. High Blood Sugar Levels
One of the primary causes of nephropathy diabetic is prolonged exposure to high blood sugar levels. When blood glucose remains elevated over time, it can damage the blood vessels in the kidneys, impairing their ability to filter waste effectively. This damage can lead to a gradual decline in kidney function.
2. High Blood Pressure
Hypertension, or high blood pressure, is another significant risk factor. It can exacerbate kidney damage in individuals with diabetes. The combination of high blood sugar and high blood pressure creates a vicious cycle that accelerates the progression of nephropathy diabetic.
3. Genetic Predisposition
Genetics also play a role in the development of diabetic nephropathy. Individuals with a family history of kidney disease may be at a higher risk. Certain genetic markers have been identified that may increase susceptibility to kidney damage in diabetic patients.
4. Duration of Diabetes
The longer a person has diabetes, the greater their risk of developing nephropathy diabetic. Studies show that after 20 years of living with diabetes, approximately 30-40% of individuals will develop some form of kidney damage.
5. Lifestyle Factors
Unhealthy lifestyle choices can significantly increase the risk of nephropathy diabetic. Factors such as:
- Obesity: Excess body weight can lead to insulin resistance and worsen blood sugar control.
- Smoking: Tobacco use can damage blood vessels and reduce blood flow to the kidneys.
- Poor Diet: A diet high in processed foods, sugars, and unhealthy fats can contribute to obesity and poor blood sugar control.
6. Other Health Conditions
Other medical conditions can also increase the risk of developing nephropathy diabetic. These include:
- Cardiovascular Disease: Individuals with heart disease are more likely to experience kidney problems.
- High Cholesterol: Elevated cholesterol levels can contribute to the hardening of blood vessels, affecting kidney function.
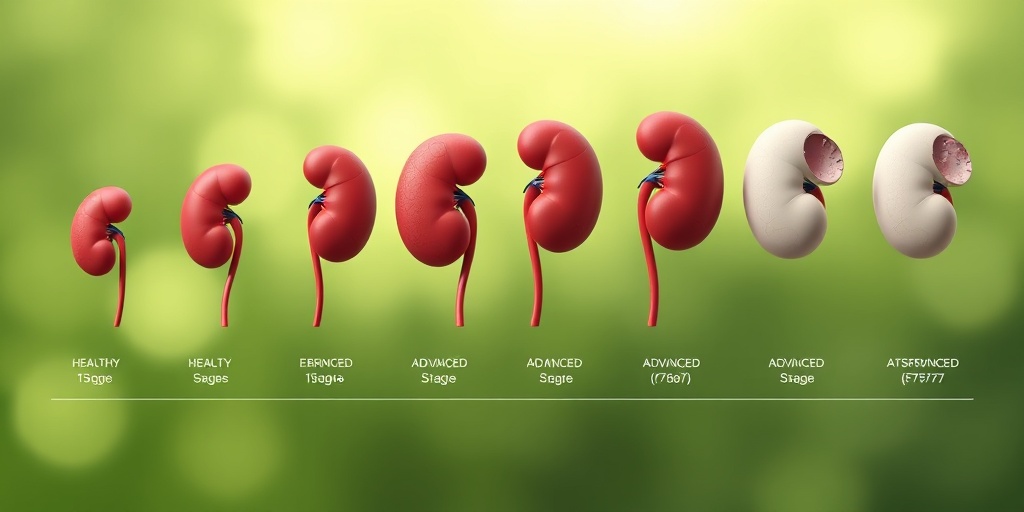
Stages of Diabetic Nephropathy
Diabetic nephropathy progresses through several stages, each characterized by specific changes in kidney function and structure. Understanding these stages can help in early detection and management of the condition.
1. Stage 1: Hyperfiltration
In the initial stage, the kidneys experience hyperfiltration, where they filter blood at an increased rate. This stage often goes unnoticed as there are typically no symptoms. However, it is a critical time for intervention to prevent further damage.
2. Stage 2: Microalbuminuria
As the condition progresses, small amounts of protein (albumin) begin to leak into the urine, a condition known as microalbuminuria. This stage may still be asymptomatic, but it indicates early kidney damage. Regular screening for protein in the urine is essential for early detection.
3. Stage 3: Macroalbuminuria
In this stage, the amount of protein in the urine increases significantly, leading to macroalbuminuria. Patients may start to experience symptoms such as swelling in the legs and feet, fatigue, and changes in urination patterns. This stage requires more aggressive management to slow progression.
4. Stage 4: Declining Kidney Function
As nephropathy diabetic advances, kidney function declines, leading to chronic kidney disease (CKD). Patients may experience more pronounced symptoms, including high blood pressure, anemia, and electrolyte imbalances. At this stage, close monitoring and treatment are crucial.
5. Stage 5: End-Stage Renal Disease (ESRD)
The final stage is end-stage renal disease (ESRD), where the kidneys can no longer function adequately. Patients may require dialysis or a kidney transplant to survive. This stage highlights the importance of early detection and management of diabetic nephropathy.
Recognizing the causes and stages of nephropathy diabetic is vital for individuals with diabetes. By managing blood sugar levels, blood pressure, and adopting a healthy lifestyle, it is possible to slow the progression of this serious condition. 🩺💙
Diagnosis of Diabetic Nephropathy
Diabetic nephropathy is a serious complication of diabetes that affects the kidneys, leading to kidney damage and, ultimately, kidney failure if left untreated. Early diagnosis is crucial for effective management and to prevent progression. Here’s how healthcare professionals diagnose this condition.
Understanding the Symptoms
Before diving into diagnostic tests, it’s essential to recognize the symptoms associated with nephropathy diabetic. Common signs include:
- Increased protein in urine (proteinuria)
- Swelling in the legs, ankles, or feet
- Fatigue and weakness
- High blood pressure
- Changes in urination patterns
Diagnostic Tests
To confirm a diagnosis of diabetic nephropathy, healthcare providers typically use a combination of the following tests:
- Urine Tests: A urine test can detect the presence of protein, which is a key indicator of kidney damage. The urine albumin-to-creatinine ratio (UACR) is often used to assess protein levels.
- Blood Tests: Blood tests measure kidney function by checking levels of creatinine and estimating the glomerular filtration rate (GFR). A declining GFR indicates worsening kidney function.
- Imaging Tests: Ultrasounds or CT scans may be used to visualize the kidneys and assess any structural abnormalities.
- Kidney Biopsy: In some cases, a biopsy may be necessary to determine the extent of kidney damage and to rule out other conditions.
ICD Codes for Diabetic Nephropathy
For medical billing and documentation, diabetic nephropathy is classified under specific ICD codes. The ICD-10 code for diabetic nephropathy is E11.21, while the ICD-9 code is 250.40. These codes help healthcare providers accurately document the condition for treatment and insurance purposes.
Treatment Options Available
Once diagnosed, managing diabetic nephropathy involves a multifaceted approach aimed at slowing the progression of kidney damage and addressing the underlying diabetes. Here are the primary treatment options available:
Medications
Several medications can help manage diabetic nephropathy:
- Angiotensin-Converting Enzyme (ACE) Inhibitors: These medications help lower blood pressure and reduce proteinuria, protecting kidney function.
- Angiotensin II Receptor Blockers (ARBs): Similar to ACE inhibitors, ARBs also help manage blood pressure and provide kidney protection.
- Diuretics: These can help reduce fluid retention and lower blood pressure.
- Glucose-Lowering Medications: Controlling blood sugar levels is crucial. Medications like metformin or insulin therapy may be prescribed.
Lifestyle Modifications
In addition to medications, lifestyle changes play a vital role in managing diabetic nephropathy:
- Diet: A balanced diet low in sodium, saturated fats, and processed sugars can help manage blood pressure and blood sugar levels. Consider consulting a dietitian for personalized meal planning.
- Regular Exercise: Engaging in regular physical activity can improve overall health and help control blood sugar levels.
- Weight Management: Maintaining a healthy weight is essential for reducing the risk of complications.
- Avoiding Tobacco and Limiting Alcohol: Smoking and excessive alcohol consumption can worsen kidney function.
Monitoring and Follow-Up
Regular follow-up appointments with healthcare providers are crucial for monitoring kidney function and adjusting treatment plans as necessary. Routine blood and urine tests will help track the progression of nephropathy and the effectiveness of treatment.
In summary, early diagnosis and a comprehensive treatment plan are key to managing nephropathy diabetic. By understanding the symptoms, undergoing appropriate tests, and adhering to treatment options, individuals can significantly improve their quality of life and protect their kidney health. 🌟
Managing Diabetic Nephropathy
Diabetic nephropathy is a serious complication of diabetes that affects the kidneys, leading to a gradual decline in kidney function. As the kidneys become less effective at filtering waste from the blood, it can result in severe health issues. Understanding how to manage this condition is crucial for those living with diabetes. Here, we’ll explore effective strategies for managing diabetic nephropathy.
Understanding the Stages of Diabetic Nephropathy
Diabetic nephropathy progresses through several stages, each with distinct characteristics:
- Stage 1: Kidney damage occurs, but kidney function remains normal. This stage is often asymptomatic.
- Stage 2: Mild reduction in kidney function is observed, with slight increases in protein in the urine.
- Stage 3: Moderate kidney damage leads to more significant proteinuria and a noticeable decline in kidney function.
- Stage 4: Severe kidney damage occurs, with significant symptoms and complications arising.
- Stage 5: End-stage renal disease (ESRD) requires dialysis or kidney transplantation.
Recognizing these stages can help in early intervention and management of diabetic nephropathy.
Regular Monitoring and Diagnosis
Regular check-ups are essential for anyone with diabetes. Monitoring kidney function through blood tests (like serum creatinine) and urine tests (to check for protein) can help detect diabetic nephropathy early. The ICD-10 code for diabetic nephropathy is E11.21, which is used for medical billing and documentation purposes.
Medications and Treatments
Managing diabetic nephropathy often involves a combination of medications and lifestyle changes. Here are some common treatment options:
- Angiotensin-converting enzyme (ACE) inhibitors: These medications help lower blood pressure and reduce proteinuria.
- Angiotensin II receptor blockers (ARBs): Similar to ACE inhibitors, ARBs also protect kidney function.
- Diuretics: These can help manage fluid retention and high blood pressure.
- Blood sugar control medications: Keeping blood sugar levels within target ranges is crucial for preventing further kidney damage.
Always consult with a healthcare provider to determine the best treatment plan tailored to individual needs.
Preventive Measures and Lifestyle Changes
Preventing the progression of diabetic nephropathy is possible through proactive lifestyle changes and preventive measures. Here are some effective strategies:
Healthy Eating Habits
Nutrition plays a vital role in managing diabetes and protecting kidney health. Consider the following dietary tips:
- Limit sodium intake: Reducing salt can help control blood pressure.
- Choose heart-healthy foods: Incorporate fruits, vegetables, whole grains, and lean proteins into your diet.
- Monitor protein consumption: While protein is essential, excessive intake can strain the kidneys.
Consulting a registered dietitian can provide personalized dietary recommendations.
Regular Physical Activity
Engaging in regular physical activity can help manage blood sugar levels and improve overall health. Aim for at least 150 minutes of moderate aerobic exercise each week, such as:
- Walking 🚶♂️
- Swimming 🏊♀️
- Cycling 🚴♂️
Incorporating strength training exercises at least twice a week can also be beneficial.
Maintaining a Healthy Weight
Being overweight can increase the risk of complications from diabetes, including nephropathy. Achieving and maintaining a healthy weight through diet and exercise can significantly reduce this risk.
Regular Health Check-ups
Frequent visits to your healthcare provider for monitoring blood pressure, blood sugar levels, and kidney function are essential. Early detection of any issues can lead to timely interventions, potentially slowing the progression of diabetic nephropathy.
In conclusion, managing diabetic nephropathy requires a comprehensive approach that includes medical treatment, lifestyle changes, and regular monitoring. By taking proactive steps, individuals can significantly improve their quality of life and reduce the risk of severe complications. 🌟

Frequently Asked Questions about Nephropathy Diabetic
What is Nephropathy Diabetic?
Nephropathy Diabetic is a type of kidney damage that occurs as a complication of diabetes. It is characterized by the gradual loss of kidney function due to high blood sugar levels over time. This condition can lead to serious health issues if not managed properly.
What are the stages of Nephropathy Diabetic?
Nephropathy Diabetic progresses through several stages:
- Stage 1: Normal kidney function with increased kidney size and hyperfiltration.
- Stage 2: Mild kidney damage with slight increase in protein in the urine.
- Stage 3: Moderate kidney damage with more significant proteinuria and decreased kidney function.
- Stage 4: Severe kidney damage with significant loss of kidney function.
- Stage 5: End-stage renal disease requiring dialysis or kidney transplant.
How is Nephropathy Diabetic diagnosed?
Diagnosis of Nephropathy Diabetic typically involves:
- Urine tests to check for protein levels.
- Blood tests to assess kidney function.
- Imaging tests to evaluate kidney structure.
What are the treatment options for Nephropathy Diabetic?
Treatment for Nephropathy Diabetic focuses on managing diabetes and protecting kidney function. Options include:
- Controlling blood sugar levels through diet, exercise, and medication.
- Using medications such as ACE inhibitors or ARBs to reduce proteinuria.
- Regular monitoring of kidney function.
Can Nephropathy Diabetic be prevented?
While not all cases of Nephropathy Diabetic can be prevented, maintaining good blood sugar control and regular check-ups can significantly reduce the risk. Lifestyle changes such as a healthy diet and regular exercise are also beneficial.
Where can I find more information on Nephropathy Diabetic?
For more detailed information, you can refer to resources such as:
- Medical journals on nephrology and diabetes.
- Online databases like NCBI for research articles.
- Educational PDFs and guides on Nephropathy Diabetic.
Is there a specific ICD code for Nephropathy Diabetic?
Yes, Nephropathy Diabetic is classified under specific ICD codes. For instance, the ICD-10 code for diabetic nephropathy is E11.21. It is important to consult healthcare professionals for accurate coding and documentation.
What is the pathophysiology of Nephropathy Diabetic?
The pathophysiology of Nephropathy Diabetic involves complex mechanisms including:
- Hyperglycemia leading to glomerular damage.
- Increased pressure in the kidneys due to high blood sugar.
- Inflammation and fibrosis contributing to kidney dysfunction.
How does Nephropathy Diabetic affect overall health?
Nephropathy Diabetic can lead to various complications, including:
- Increased risk of cardiovascular diseases.
- Progression to end-stage renal disease.
- Potential need for dialysis or kidney transplant.
Are there any lifestyle changes that can help manage Nephropathy Diabetic?
Yes, adopting a healthy lifestyle can greatly assist in managing Nephropathy Diabetic. Consider the following:
- Eating a balanced diet low in sodium and saturated fats.
- Engaging in regular physical activity.
- Avoiding smoking and limiting alcohol consumption.
If you have more questions or need further assistance, feel free to reach out! 😊




