What Is Shock?
Shock is a critical medical condition that occurs when the body is not getting enough blood flow, leading to a lack of oxygen and nutrients to vital organs. This can result in serious complications and, if not treated promptly, can be life-threatening. Understanding shock is essential for recognizing its symptoms and knowing how to respond effectively.
In simple terms, shock can be described as a state of acute circulatory failure. It can happen due to various reasons, including trauma, severe infections, allergic reactions, or heart problems. When the body experiences shock, it triggers a series of physiological responses aimed at preserving life, but these responses can also lead to further complications if not managed properly.
Signs and Symptoms of Shock
Recognizing the signs of shock is crucial for timely intervention. Common symptoms include:
- Rapid heartbeat: The heart races to compensate for low blood flow.
- Weak pulse: A weak or thready pulse can indicate poor circulation.
- Pale or clammy skin: Blood is diverted from the skin to vital organs.
- Confusion or disorientation: The brain may not receive enough oxygen.
- Shortness of breath: Difficulty breathing can occur as the body struggles to get enough oxygen.
- Low blood pressure: A significant drop in blood pressure is a hallmark of shock.
If you or someone you know exhibits these symptoms, it is vital to seek medical attention immediately. Early recognition and treatment can significantly improve outcomes.
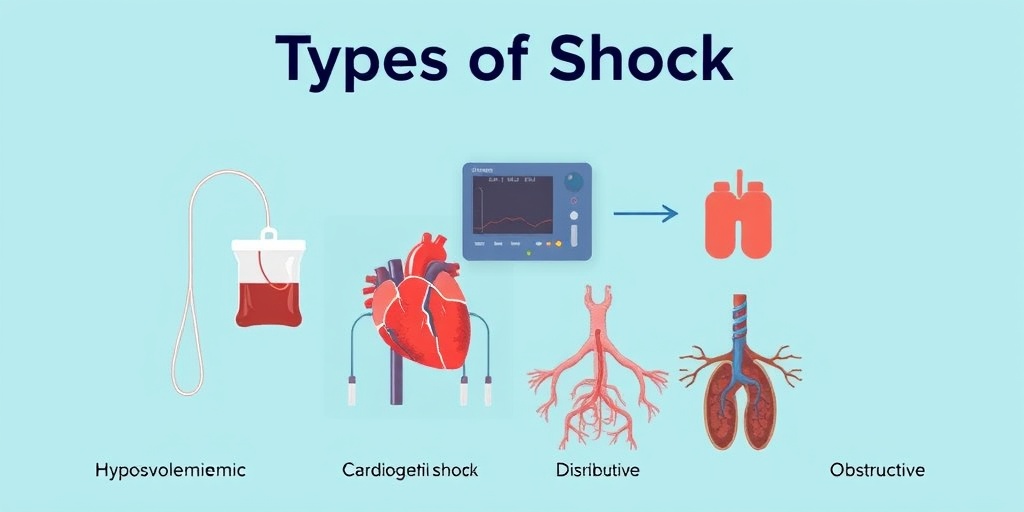
Types of Shock
Shock is not a one-size-fits-all condition; it can be classified into several types based on its underlying cause. Understanding these types can help in identifying the appropriate treatment and management strategies.
1. Hypovolemic Shock
Hypovolemic shock occurs when there is a significant loss of blood volume, often due to trauma, severe dehydration, or internal bleeding. The body struggles to maintain adequate blood flow to organs, leading to the symptoms mentioned earlier. Treatment typically involves fluid replacement and addressing the underlying cause of the volume loss.
2. Cardiogenic Shock
This type of shock arises from the heart’s inability to pump blood effectively, often due to a heart attack or severe heart failure. Patients may experience chest pain, shortness of breath, and extreme fatigue. Treatment focuses on improving heart function and may include medications, surgery, or other interventions.
3. Distributive Shock
Distributive shock is characterized by abnormal distribution of blood flow in the smallest blood vessels. This type includes septic shock (caused by severe infections), anaphylactic shock (a severe allergic reaction), and neurogenic shock (resulting from spinal cord injuries). Each subtype requires specific treatment approaches, such as antibiotics for septic shock or epinephrine for anaphylaxis.
4. Obstructive Shock
Obstructive shock occurs when blood flow is obstructed, often due to conditions like pulmonary embolism or cardiac tamponade. This type of shock requires immediate medical intervention to relieve the obstruction and restore normal blood flow.
5. Septic Shock
Septic shock is a severe and life-threatening response to infection, leading to systemic inflammation and organ dysfunction. It is crucial to recognize and treat septic shock promptly, as it can progress rapidly. Treatment typically involves antibiotics, intravenous fluids, and sometimes vasopressors to stabilize blood pressure.
Conclusion
Understanding shock and its various types is essential for recognizing the signs and symptoms that require immediate medical attention. If you suspect someone is experiencing shock, do not hesitate to call for help. For more information on health-related topics, including shock and its management, visit Yesil Health AI, a valuable resource for evidence-based health answers.
Remember, timely intervention can save lives! Stay informed and be prepared to act in emergencies. 🚑
Shock Symptoms
Shock is a serious medical condition that occurs when the body is not getting enough blood flow, leading to a lack of oxygen and nutrients in vital organs. Recognizing the symptoms of shock is crucial for timely intervention and treatment. Here are some common symptoms to watch for:
Physical Symptoms
- Pale or Clammy Skin: One of the first signs of shock is a noticeable change in skin color and temperature. The skin may appear pale, cool, or clammy to the touch.
- Rapid Heart Rate: The heart works harder to pump blood to vital organs, resulting in a fast or irregular heartbeat.
- Weak Pulse: Despite the rapid heart rate, the pulse may feel weak or thready, indicating that blood flow is compromised.
- Shallow Breathing: Breathing may become rapid and shallow as the body struggles to get enough oxygen.
- Confusion or Disorientation: A lack of blood flow to the brain can lead to confusion, disorientation, or even loss of consciousness.
Emotional and Cognitive Symptoms
- Anxiety or Restlessness: Individuals in shock may feel anxious or restless, often unable to sit still.
- Feeling of Impending Doom: Many people report a sense of impending doom or fear, which can be a psychological response to the body’s distress.
- Loss of Consciousness: In severe cases, shock can lead to fainting or loss of consciousness, requiring immediate medical attention.
Recognizing these symptoms early can be life-saving. If you or someone else exhibits signs of shock, it is essential to seek medical help immediately. 🚑
Causes of Shock
Understanding the causes of shock is vital for prevention and treatment. Shock can result from various factors, and identifying the underlying cause is crucial for effective management. Here are some common causes:
Hypovolemic Shock
This type of shock occurs when there is a significant loss of blood or fluids in the body. Common causes include:
- Severe Bleeding: Trauma, surgery, or internal bleeding can lead to a rapid loss of blood volume.
- Dehydration: Excessive vomiting, diarrhea, or sweating can cause dehydration, leading to hypovolemic shock.
Cardiogenic Shock
Cardiogenic shock occurs when the heart is unable to pump enough blood to meet the body’s needs. Causes include:
- Heart Attack: A heart attack can damage the heart muscle, impairing its ability to pump effectively.
- Heart Failure: Chronic heart conditions can lead to cardiogenic shock, especially during periods of increased stress on the heart.
Distributive Shock
This type of shock is characterized by widespread vasodilation, leading to inadequate blood flow. Common causes include:
- Septic Shock: A severe infection can cause the body to go into shock as it responds to the infection.
- Anaphylactic Shock: A severe allergic reaction can lead to a sudden drop in blood pressure and shock.
Obstructive Shock
Obstructive shock occurs when blood flow is obstructed, preventing adequate circulation. Causes include:
- Pulmonary Embolism: A blood clot in the lungs can obstruct blood flow, leading to shock.
- Tension Pneumothorax: Air trapped in the chest cavity can compress the lungs and heart, causing shock.
Understanding these causes can help in recognizing the risk factors associated with shock. If you suspect someone is experiencing shock, it is crucial to act quickly and seek medical assistance. Remember, timely intervention can make all the difference! 💔

Risk Factors for Shock
Shock is a critical medical condition that occurs when the body does not receive enough blood flow, leading to a lack of oxygen and nutrients in vital organs. Understanding the risk factors for shock is essential for prevention and early intervention. Here, we will explore various factors that can increase the likelihood of experiencing shock.
1. Medical Conditions
Several underlying medical conditions can predispose individuals to shock. These include:
- Heart Problems: Conditions such as heart attack, congestive heart failure, or arrhythmias can impair the heart’s ability to pump blood effectively.
- Severe Infections: Sepsis, a life-threatening response to infection, can lead to septic shock, where the body goes into overdrive to fight infection, causing a drop in blood pressure.
- Severe Allergic Reactions: Anaphylaxis can cause an extreme drop in blood pressure and lead to anaphylactic shock.
- Severe Blood Loss: Trauma, surgery, or gastrointestinal bleeding can result in hypovolemic shock due to significant blood loss.
2. Lifestyle Factors
Certain lifestyle choices can also contribute to the risk of shock:
- Substance Abuse: Excessive alcohol consumption or drug use can lead to dehydration and cardiovascular issues, increasing the risk of shock.
- Poor Nutrition: A diet lacking essential nutrients can weaken the immune system and overall health, making one more susceptible to conditions that can lead to shock.
- Inactivity: A sedentary lifestyle can contribute to obesity and cardiovascular diseases, which are significant risk factors for shock.
3. Environmental Factors
Environmental conditions can also play a role in the risk of shock:
- Extreme Temperatures: Exposure to extreme heat or cold can lead to heat stroke or hypothermia, both of which can result in shock.
- High Altitudes: Rapid ascent to high altitudes can cause altitude sickness, which may lead to shock in susceptible individuals.
4. Age and Gender
Age and gender can influence the risk of shock:
- Older Adults: Aging can lead to a decline in cardiovascular health, making older adults more vulnerable to shock.
- Gender Differences: Some studies suggest that men may be at a higher risk for certain types of shock, such as cardiogenic shock, due to higher rates of heart disease.
Shock Diagnosis
Diagnosing shock promptly is crucial for effective treatment. Medical professionals use a combination of clinical evaluation and diagnostic tests to determine the presence and type of shock. Here’s how the diagnosis process typically unfolds:
1. Clinical Assessment
The first step in diagnosing shock involves a thorough clinical assessment. Healthcare providers will:
- Evaluate Symptoms: Common symptoms of shock include rapid heartbeat, low blood pressure, confusion, pale skin, and shallow breathing.
- Check Vital Signs: Monitoring blood pressure, heart rate, and respiratory rate helps assess the severity of the condition.
- Perform a Physical Examination: A physical exam can reveal signs of shock, such as cool, clammy skin or altered mental status.
2. Diagnostic Tests
In addition to a clinical assessment, various diagnostic tests may be conducted to confirm the diagnosis and identify the underlying cause:
- Blood Tests: Blood tests can help determine oxygen levels, electrolyte balance, and the presence of infection or organ dysfunction.
- Imaging Studies: X-rays, CT scans, or ultrasounds may be used to identify internal bleeding or other issues contributing to shock.
- Electrocardiogram (ECG): An ECG can assess heart function and detect any arrhythmias that may be causing shock.
3. Identifying the Type of Shock
Shock can be classified into several types, each requiring different treatment approaches:
- Hypovolemic Shock: Caused by significant blood loss or fluid loss.
- Cardiogenic Shock: Results from the heart’s inability to pump blood effectively.
- Distributive Shock: Includes septic shock and anaphylactic shock, where blood vessels dilate excessively.
- Obstructive Shock: Occurs when blood flow is obstructed, such as in cases of pulmonary embolism.
Understanding the risk factors for shock and the diagnostic process is vital for timely intervention and treatment. If you or someone you know exhibits symptoms of shock, seek medical attention immediately. 🏥

Shock Treatment Options
Shock is a serious medical condition that occurs when the body is not getting enough blood flow, leading to a lack of oxygen and nutrients to vital organs. It can be caused by various factors, including trauma, severe infections, allergic reactions, or significant blood loss. Understanding the treatment options available for shock is crucial for timely intervention and recovery.
Types of Shock and Their Treatments
There are several types of shock, each requiring specific treatment approaches. Here are the most common types:
- Hypovolemic Shock: This type occurs due to a significant loss of blood or fluids. Treatment typically involves:
- Fluid Resuscitation: Administering intravenous (IV) fluids to restore blood volume.
- Blood Transfusions: In cases of severe blood loss, transfusions may be necessary to replace lost blood.
- Cardiogenic Shock: This occurs when the heart cannot pump enough blood to meet the body’s needs. Treatment options include:
- Medications: Drugs that improve heart function, such as inotropes, may be administered.
- Mechanical Support: Devices like intra-aortic balloon pumps can help support heart function.
- Distributive Shock: This includes septic shock, neurogenic shock, and anaphylactic shock. Treatments vary based on the cause:
- Septic Shock: Antibiotics and IV fluids are critical to combat infection.
- Anaphylactic Shock: Immediate administration of epinephrine is essential to counteract severe allergic reactions.
- Obstructive Shock: This occurs when blood flow is obstructed. Treatment may involve:
- Relieving the Obstruction: Procedures to remove blockages, such as in cases of pulmonary embolism.
Immediate First Aid for Shock
While professional medical treatment is crucial, knowing how to provide immediate first aid can save lives. Here are some steps to take:
- Call Emergency Services: Always seek professional help immediately.
- Lay the Person Down: Position them flat on their back to improve blood flow to vital organs.
- Keep Them Warm: Use a blanket to prevent hypothermia, as shock can cause body temperature to drop.
- Monitor Vital Signs: Keep an eye on their breathing and pulse until help arrives.
Preventing Shock
Prevention is always better than cure, especially when it comes to shock. While not all types of shock can be prevented, there are several strategies to minimize the risk:
Awareness and Education
Understanding the causes and symptoms of shock is vital. Being aware of the signs, such as rapid heartbeat, confusion, pale skin, and shallow breathing, can help in early detection and intervention. Educating yourself and others about the risks associated with trauma, severe allergies, and infections can also play a significant role in prevention.
Managing Chronic Conditions
For individuals with chronic health issues, such as heart disease or diabetes, managing these conditions effectively can reduce the risk of shock. Regular check-ups, adhering to prescribed medications, and maintaining a healthy lifestyle are essential steps.
Safety Measures
Implementing safety measures can help prevent accidents that may lead to shock:
- Wear Seatbelts: Always buckle up in vehicles to reduce the risk of injury during accidents.
- Use Protective Gear: When engaging in sports or hazardous activities, wear appropriate protective equipment.
- Practice Food Safety: Properly handle and cook food to prevent foodborne illnesses that can lead to septic shock.
Emergency Preparedness
Being prepared for emergencies can make a significant difference. Consider the following:
- First Aid Training: Taking a first aid course can equip you with the skills needed to respond effectively in emergencies.
- Emergency Kit: Keep a well-stocked emergency kit at home and in your car, including items like bandages, antiseptics, and medications.
By understanding shock and its treatment options, as well as taking proactive steps to prevent it, you can significantly improve outcomes in critical situations. Remember, awareness and preparedness are key! 💪

Frequently Asked Questions about Shock
What is shock?
Shock is a medical emergency condition that occurs when the body is not getting enough blood flow, leading to a lack of oxygen and nutrients to vital organs. It can result from various causes, including trauma, severe infections, or allergic reactions.
What are the symptoms of shock?
- Rapid heartbeat
- Pale or clammy skin
- Weak pulse
- Confusion or disorientation
- Shortness of breath
- Extreme thirst
What types of shock are there?
There are several types of shock, including:
- Hypovolemic shock: Caused by severe blood loss or dehydration.
- Cardiogenic shock: Results from the heart’s inability to pump blood effectively.
- Distributive shock: Includes septic shock, anaphylactic shock, and neurogenic shock, where blood vessels dilate excessively.
- Obstructive shock: Occurs when blood flow is obstructed, such as in cases of pulmonary embolism.
How is shock treated?
Treatment for shock depends on its cause but may include:
- Administering fluids and medications to stabilize blood pressure.
- Providing oxygen to improve oxygenation.
- Addressing the underlying cause, such as treating an infection or stopping bleeding.
Can shock be prevented?
While not all cases of shock can be prevented, certain measures can reduce the risk, such as:
- Staying hydrated, especially in hot weather.
- Managing chronic health conditions effectively.
- Wearing seatbelts and following safety protocols to prevent trauma.
What should I do if someone is in shock?
If you suspect someone is experiencing shock, it is crucial to seek emergency medical help immediately. While waiting for help:
- Lay the person down and elevate their legs if possible.
- Keep them warm and comfortable.
- Avoid giving them food or drink.
What is the difference between shock and a shock absorber?
While shock refers to a medical condition, a shock absorber is a mechanical device used in vehicles to dampen the impact of bumps and vibrations on the road. They serve entirely different purposes in health and engineering.
What does the shocked emoji mean? 🤯
The shocked emoji typically represents surprise, disbelief, or astonishment. It is often used in conversations to express a strong emotional reaction to unexpected news or events.
What is culture shock? 🌍
Culture shock refers to the feelings of confusion and anxiety that people may experience when they are exposed to a new and unfamiliar culture. It can occur when traveling or moving to a different country and can involve adjusting to new social norms, languages, and customs.




