What Is HHT?
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder that affects blood vessels, leading to abnormal connections between arteries and veins. This condition is also known as Osler-Weber-Rendu syndrome. Individuals with HHT often experience a range of symptoms due to the formation of small, dilated blood vessels (telangiectasias) that can bleed easily. Understanding HHT is crucial for early diagnosis and effective management.
Understanding the Genetics of HHT
HHT is inherited in an autosomal dominant pattern, meaning that only one copy of the mutated gene from an affected parent can cause the disorder in their offspring. The genes primarily associated with HHT are:
- ENG (Endoglin) – Located on chromosome 9.
- ACVRL1 (Activin A receptor type II-like kinase 1) – Found on chromosome 12.
- SMAD4 – Linked to a more severe form of HHT.
These genes play a vital role in the development and maintenance of blood vessels, and mutations can lead to the characteristic symptoms of HHT.
How Common Is HHT?
HHT is estimated to affect approximately 1 in 5,000 individuals worldwide. However, many cases remain undiagnosed due to a lack of awareness about the condition. Early recognition and diagnosis are essential for managing symptoms and preventing complications.
HHT Symptoms
The symptoms of HHT can vary widely among individuals, and some may experience mild symptoms while others face more severe complications. Here are the most common symptoms associated with HHT:
Nosebleeds
One of the hallmark symptoms of HHT is frequent nosebleeds, which can occur spontaneously and may be difficult to control. These nosebleeds can be a significant source of discomfort and anxiety for those affected.
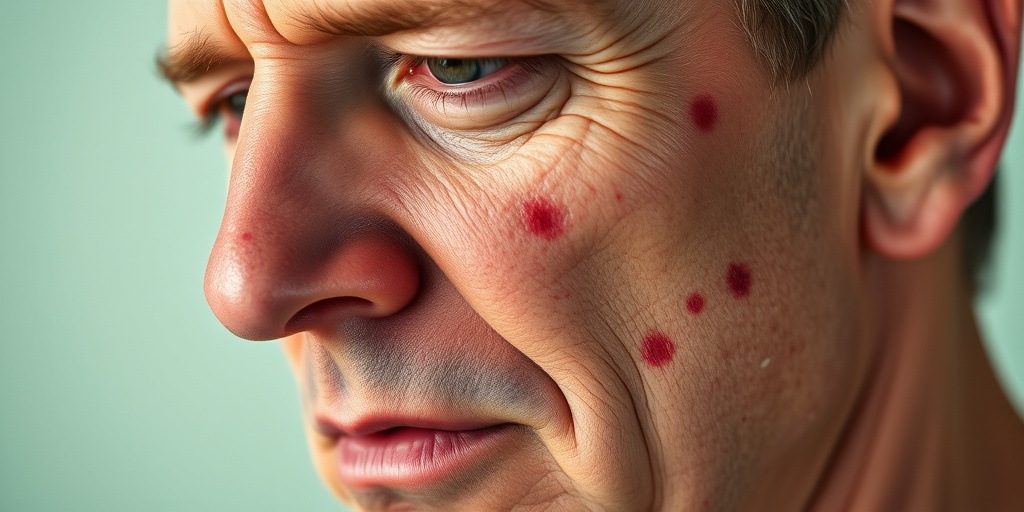
Telangiectasias
Telangiectasias are small, red or purple spots that appear on the skin and mucous membranes. They are often found on the face, hands, and inside the mouth. While these spots are usually harmless, they can bleed easily, leading to further complications.
Gastrointestinal Bleeding
Individuals with HHT may also experience gastrointestinal bleeding due to telangiectasias in the digestive tract. This can lead to symptoms such as:
- Abdominal pain
- Black or tarry stools
- Anemia due to blood loss
It is crucial to seek medical attention if gastrointestinal bleeding occurs, as it can be life-threatening.
Pulmonary Complications
HHT can also affect the lungs, leading to pulmonary arteriovenous malformations (AVMs). These abnormal connections can cause symptoms such as:
- Shortness of breath
- Fatigue
- Recurrent respiratory infections
In severe cases, pulmonary AVMs can lead to serious complications, including stroke.
Other Symptoms
In addition to the symptoms mentioned above, individuals with HHT may experience:
- Joint pain
- Vision problems due to retinal telangiectasias
- Skin changes and lesions
Recognizing these symptoms early can help in managing HHT effectively and improving the quality of life for those affected.
If you or someone you know is experiencing symptoms of HHT, it is essential to consult a healthcare professional for proper diagnosis and management. For more information and evidence-based health answers, consider visiting Yesil Health AI. They provide valuable resources to help you navigate health concerns effectively. 🌟
HHT Causes
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder that affects blood vessels, leading to abnormal connections between arteries and veins. Understanding the causes of HHT is crucial for early diagnosis and management. Let’s delve into the primary causes of this condition.
Genetic Factors
The primary cause of HHT is genetic mutations. This condition is typically inherited in an autosomal dominant pattern, meaning that only one copy of the mutated gene from an affected parent can cause the disorder in their offspring. The genes most commonly associated with HHT include:
- ENG (Endoglin): This gene is located on chromosome 9 and is responsible for the production of a protein that helps regulate blood vessel formation.
- ACVRL1 (Activin A receptor type II-like 1): Found on chromosome 12, this gene also plays a role in blood vessel development.
- SMAD4: Although less common, mutations in this gene can lead to a more severe form of HHT, often associated with other health issues.
Individuals with a family history of HHT are at a higher risk of inheriting these mutations. Genetic testing can help identify carriers of the disease, allowing for early intervention and monitoring.
Environmental Factors
While HHT is primarily a genetic disorder, certain environmental factors may exacerbate symptoms or complications. For instance, high altitudes can increase the risk of bleeding episodes due to lower oxygen levels, which may affect blood vessel integrity. Additionally, smoking and exposure to pollutants can worsen vascular health, potentially leading to more severe manifestations of HHT.
Understanding the Symptoms
Recognizing the symptoms of HHT can help in understanding its causes. Common symptoms include:
- Nosebleeds: Frequent and spontaneous nosebleeds are often one of the first signs of HHT.
- Skin Lesions: Telangiectasias, or small red spots, may appear on the skin, particularly on the face and hands.
- Gastrointestinal Bleeding: This can occur due to abnormal blood vessels in the digestive tract.
Being aware of these symptoms can prompt individuals to seek medical advice, leading to earlier diagnosis and management of the condition.
HHT Diagnosis
Diagnosing Hereditary Hemorrhagic Telangiectasia (HHT) involves a combination of clinical evaluation, family history assessment, and specific diagnostic tests. Early diagnosis is essential for effective management and reducing complications associated with the disorder.
Clinical Evaluation
The first step in diagnosing HHT typically involves a thorough clinical evaluation by a healthcare professional. During this evaluation, the doctor will:
- Review the patient’s medical history, including any family history of HHT.
- Conduct a physical examination to check for signs such as telangiectasias on the skin and mucous membranes.
- Assess for any symptoms related to bleeding, such as frequent nosebleeds or gastrointestinal issues.
Genetic Testing
If HHT is suspected based on clinical evaluation, genetic testing may be recommended. This testing can confirm the presence of mutations in the ENG, ACVRL1, or SMAD4 genes. Genetic counseling is often advised for individuals undergoing testing, as it can provide valuable information about the implications of the results for the patient and their family.
Imaging Studies
In some cases, imaging studies may be necessary to assess the extent of vascular malformations. Common imaging techniques include:
- Magnetic Resonance Imaging (MRI): This can help visualize blood vessels in the brain and other organs.
- Ultrasound: Useful for detecting vascular malformations in the liver and other abdominal organs.
- Angiography: A specialized imaging technique that provides detailed images of blood vessels.
These imaging studies can help determine the severity of the condition and guide treatment options.
Importance of Early Diagnosis
Early diagnosis of HHT is crucial for managing symptoms and preventing complications. Regular monitoring and follow-up care can significantly improve the quality of life for individuals with HHT. By understanding the causes and diagnostic processes, patients and families can take proactive steps toward managing this condition effectively. 🌟
HHT Treatment Options
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder that affects blood vessels, leading to abnormal connections between arteries and veins. This condition can result in various symptoms, including nosebleeds, gastrointestinal bleeding, and anemia. Fortunately, there are several treatment options available to manage HHT effectively. Let’s explore these options in detail.
1. Medical Management
For many individuals with HHT, medical management is the first line of defense. This approach focuses on controlling symptoms and preventing complications. Here are some common medical treatments:
- Iron Supplements: Due to frequent bleeding, many patients experience anemia. Iron supplements can help replenish iron levels and improve energy.
- Desmopressin: This medication can help reduce the frequency of nosebleeds by promoting the release of clotting factors.
- Antibiotics: In cases where patients are at risk of infections, especially after procedures, antibiotics may be prescribed.
2. Minimally Invasive Procedures
For more severe cases of HHT, minimally invasive procedures can be effective in managing symptoms and reducing complications. These procedures include:
- Laser Therapy: This technique uses focused light to treat abnormal blood vessels, reducing the risk of bleeding.
- Embolization: This procedure involves blocking blood flow to problematic blood vessels, which can help prevent bleeding episodes.
- Endoscopic Treatments: For gastrointestinal bleeding, endoscopic techniques can be used to cauterize or seal off bleeding vessels.
3. Surgical Interventions
In some cases, surgical intervention may be necessary. Surgery can be considered for patients with severe complications or those who do not respond to other treatments. Options include:
- Resection of Affected Organs: If HHT leads to significant complications in organs like the liver or lungs, surgical removal of affected tissue may be required.
- Transplantation: In extreme cases, organ transplantation may be necessary, particularly for patients with liver involvement.
4. Genetic Counseling
Since HHT is a genetic disorder, genetic counseling is an essential component of treatment. This service helps patients and their families understand the condition, its inheritance patterns, and the implications for future generations. Genetic counselors can provide valuable information about:
- Testing options for family members
- Management strategies for those at risk
- Support resources available for families
HHT Complications
While HHT can be managed effectively, it is crucial to be aware of potential complications that may arise from the condition. Understanding these complications can help patients and healthcare providers take proactive measures to mitigate risks.
1. Anemia
One of the most common complications of HHT is anemia, often resulting from chronic bleeding. Patients may experience fatigue, weakness, and shortness of breath. Regular monitoring of hemoglobin levels and appropriate management, such as iron supplementation, is essential to prevent severe anemia.
2. Pulmonary Arteriovenous Malformations (PAVMs)
PAVMs are abnormal connections between arteries and veins in the lungs, which can lead to serious complications, including:
- Hypoxemia: Reduced oxygen levels in the blood can cause fatigue and shortness of breath.
- Stroke: PAVMs can allow blood clots to bypass the lungs, increasing the risk of stroke.
3. Gastrointestinal Bleeding
Patients with HHT may also experience gastrointestinal bleeding, which can be life-threatening. This bleeding often occurs due to telangiectasias in the gastrointestinal tract. Regular screening and endoscopic interventions can help manage this complication effectively.
4. Liver Involvement
Some individuals with HHT may develop liver complications, including hepatic arteriovenous malformations. These can lead to portal hypertension and liver dysfunction, necessitating careful monitoring and potential surgical intervention.
5. Psychological Impact
The chronic nature of HHT and its associated complications can take a toll on mental health. Patients may experience anxiety, depression, or social isolation. It is essential to address these psychological aspects through support groups, counseling, and open communication with healthcare providers.
In conclusion, while HHT presents various challenges, understanding treatment options and potential complications can empower patients to manage their condition effectively. Regular follow-ups with healthcare professionals and a proactive approach to symptom management are key to living well with HHT. 🌟

HHT Management Strategies
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder that affects blood vessel formation, leading to abnormal blood vessels that can cause bleeding. Managing HHT effectively requires a comprehensive approach that includes medical treatment, lifestyle adjustments, and regular monitoring. Here are some key strategies for managing HHT:
1. Regular Medical Check-ups
One of the most crucial aspects of managing HHT is maintaining regular appointments with healthcare providers who specialize in this condition. These check-ups can help monitor the progression of the disease and identify any complications early on. Routine blood tests and imaging studies may be recommended to assess the health of your blood vessels.
2. Treatment Options
There are several treatment options available for managing HHT symptoms:
- Laser Therapy: This is often used to treat bleeding lesions on the skin or mucous membranes.
- Embolization: A minimally invasive procedure that blocks blood flow to problematic blood vessels, reducing bleeding.
- Iron Supplements: For those experiencing anemia due to chronic bleeding, iron supplements can help restore healthy iron levels.
- Medications: Some patients may benefit from medications that help manage symptoms or reduce bleeding episodes.
3. Lifestyle Modifications
Making certain lifestyle changes can significantly improve the quality of life for individuals with HHT:
- Stay Hydrated: Drinking plenty of water can help maintain overall health and support blood circulation.
- Avoid Strenuous Activities: High-impact sports or activities that increase the risk of injury should be avoided to prevent bleeding.
- Healthy Diet: A balanced diet rich in vitamins and minerals can support overall health and help manage symptoms.
4. Education and Awareness
Understanding HHT is vital for effective management. Patients and their families should educate themselves about the condition, its symptoms, and potential complications. This knowledge empowers individuals to make informed decisions about their health and seek timely medical attention when necessary.
HHT Support and Resources
Living with HHT can be challenging, but numerous resources and support systems are available to help individuals and families navigate this condition. Here are some valuable resources:
1. HHT Organizations
Several organizations focus on HHT awareness, research, and support:
- The HHT Foundation: This organization provides information, resources, and support for individuals with HHT and their families. They also fund research to improve treatment options.
- HHT International: A global network that connects patients, families, and healthcare providers to share information and experiences related to HHT.
2. Support Groups
Connecting with others who understand the challenges of living with HHT can be incredibly beneficial. Support groups offer a safe space to share experiences, discuss coping strategies, and provide emotional support. Many organizations host both in-person and online support groups.
3. Educational Resources
Access to educational materials can help patients and families better understand HHT. Websites, brochures, and webinars can provide valuable information about managing the condition, treatment options, and the latest research findings.
4. Mental Health Support
Living with a chronic condition like HHT can take a toll on mental health. Seeking support from mental health professionals can be an essential part of managing the emotional aspects of the disease. Therapists and counselors can help individuals cope with anxiety, depression, or stress related to HHT.
In conclusion, managing HHT effectively involves a combination of medical treatment, lifestyle changes, and support from healthcare providers and community resources. By staying informed and connected, individuals with HHT can lead fulfilling lives while navigating the challenges of this condition. 🌟

Frequently Asked Questions about HHT
What is HHT?
HHT, or Hereditary Hemorrhagic Telangiectasia, is a genetic disorder that leads to abnormal blood vessel formation. This condition can cause various symptoms, including frequent nosebleeds, skin lesions, and gastrointestinal bleeding.
What are the symptoms of HHT?
- Nosebleeds: Frequent and spontaneous nosebleeds are one of the most common symptoms.
- Telangiectasias: Small red or purple spots on the skin or mucous membranes.
- Gastrointestinal bleeding: This can occur due to abnormal blood vessels in the digestive tract.
- Shortness of breath: This may result from anemia caused by bleeding.
How is HHT diagnosed?
Diagnosis of HHT typically involves a combination of clinical evaluation, family history assessment, and imaging studies. Genetic testing may also be conducted to confirm the diagnosis.
What treatments are available for HHT?
While there is no cure for HHT, treatments focus on managing symptoms and preventing complications. Options may include:
- Laser therapy: Used to treat telangiectasias.
- Iron supplements: To manage anemia resulting from bleeding.
- Blood transfusions: In severe cases of anemia.
Can HHT be inherited?
Yes, HHT is an inherited condition, typically passed down in an autosomal dominant pattern. This means that an affected individual has a 50% chance of passing the disorder to each child.
Where can I find more information about HHT?
For more detailed information about HHT, consider visiting reputable health websites or organizations dedicated to genetic disorders. You can also consult with a healthcare professional who specializes in genetic conditions.
Is there support available for individuals with HHT?
Yes, there are support groups and organizations that provide resources and community support for individuals and families affected by HHT. Connecting with others who understand the condition can be incredibly beneficial.




