What Is Shock Lung?
Shock lung, also known as acute respiratory distress syndrome (ARDS), is a serious condition that affects the lungs and can lead to respiratory failure. It occurs when the lungs become severely inflamed and filled with fluid, making it difficult for oxygen to reach the bloodstream. This condition can arise from various causes, including trauma, pneumonia, sepsis, and other critical illnesses.
Understanding shock lung is crucial, as it can develop rapidly and requires immediate medical attention. The term “shock lung” is often used interchangeably with ARDS, but it specifically refers to the lung complications that arise from systemic shock, such as septic shock or hypovolemic shock. In these situations, the body’s response to injury or infection can lead to widespread inflammation, affecting lung function.
How Does Shock Lung Develop?
Shock lung typically develops in stages, often following a precipitating event. Here’s a brief overview of the process:
- Initial Injury: An event such as trauma, infection, or severe illness triggers an inflammatory response.
- Inflammation: The body releases chemicals that cause inflammation in the lungs, leading to increased permeability of the blood vessels.
- Fluid Accumulation: Fluid leaks into the alveoli (air sacs in the lungs), impairing gas exchange.
- Respiratory Failure: As the lungs struggle to function, oxygen levels in the blood drop, leading to respiratory distress.
Shock lung is characterized by a rapid onset of symptoms and can progress quickly, making early recognition and treatment essential. If you suspect someone may be experiencing shock lung, it’s vital to seek medical help immediately.
Shock Lung Symptoms
The symptoms of shock lung can vary depending on the underlying cause and the severity of the condition. However, there are common signs that may indicate the presence of shock lung:
Common Symptoms
- Shortness of Breath: Patients often experience difficulty breathing, which may worsen over time.
- Rapid Breathing: Increased respiratory rate is a common response as the body attempts to compensate for low oxygen levels.
- Cough: A persistent cough may develop, sometimes producing mucus or phlegm.
- Chest Pain: Discomfort or pain in the chest can occur, particularly during breathing or coughing.
- Fatigue: General weakness and fatigue are common as the body struggles to get enough oxygen.
- Confusion or Disorientation: Low oxygen levels can affect brain function, leading to confusion or altered mental status.
When to Seek Medical Attention
If you or someone you know is experiencing symptoms of shock lung, it’s crucial to seek medical attention promptly. Early intervention can significantly improve outcomes and reduce the risk of complications. Symptoms such as severe shortness of breath, persistent chest pain, or confusion should never be ignored.
Conclusion
Shock lung is a serious condition that requires immediate medical attention. Understanding its symptoms and the underlying mechanisms can help in recognizing the signs early. If you want to learn more about shock lung and related health topics, consider visiting Yesil Health AI for evidence-based health answers. Remember, timely intervention can save lives! 🌟
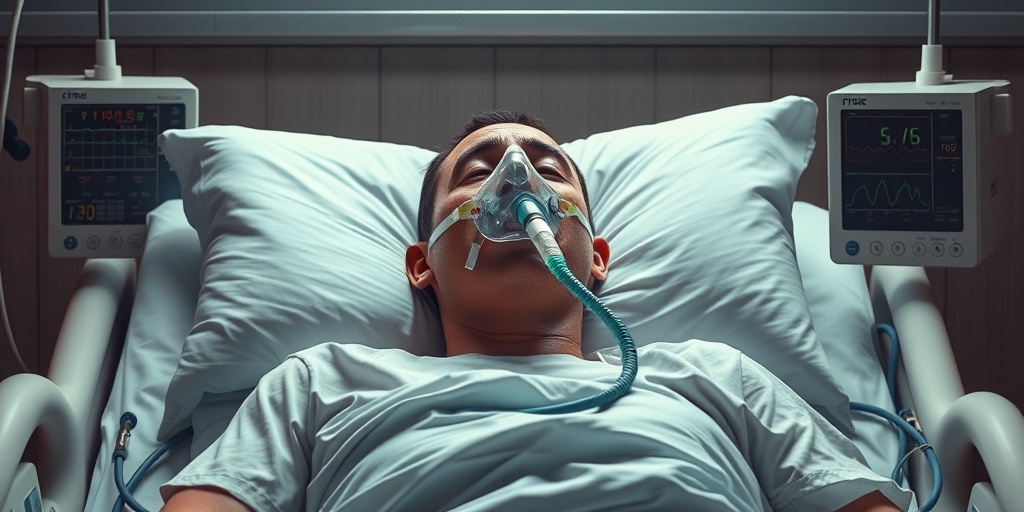
Causes of Shock Lung
Shock lung, also known as acute respiratory distress syndrome (ARDS), is a serious condition that affects the lungs and can lead to respiratory failure. Understanding the causes of shock lung is crucial for prevention and timely treatment. Here are some of the primary causes:
1. Pneumonia
Pneumonia is one of the most common causes of shock lung. This infection can lead to inflammation in the lungs, causing fluid to accumulate in the air sacs. As a result, oxygen exchange becomes impaired, leading to severe respiratory distress.
2. Sepsis
Sepsis, a life-threatening response to infection, can also trigger shock lung. When the body fights an infection, it releases chemicals that can cause widespread inflammation. This inflammation can damage the lungs, leading to ARDS.
3. Trauma
Physical trauma, such as from a car accident or a fall, can cause shock lung. Injuries to the chest can lead to lung contusions or direct damage to lung tissue, resulting in fluid buildup and impaired oxygenation.
4. Aspiration
Aspiration occurs when food, liquid, or vomit enters the lungs. This can lead to aspiration pneumonia, which can quickly progress to shock lung if not treated promptly. The foreign material can irritate lung tissue and cause inflammation.
5. Inhalation of Harmful Substances
Inhaling toxic substances, such as smoke or chemical fumes, can severely damage lung tissue. This damage can lead to inflammation and fluid accumulation, resulting in shock lung.
6. Blood Transfusion-Related Acute Lung Injury (TRALI)
TRALI is a rare but serious complication that can occur after a blood transfusion. It is characterized by acute lung injury and can lead to shock lung. The exact mechanism is not fully understood, but it is believed to involve an immune response to the transfused blood.
Risk Factors for Shock Lung
Identifying the risk factors for shock lung can help in early detection and prevention. Here are some key risk factors to consider:
1. Age
Older adults are at a higher risk for developing shock lung. As we age, our immune system becomes less effective, making it harder to fight off infections that can lead to ARDS.
2. Pre-existing Health Conditions
Individuals with pre-existing health conditions, such as chronic obstructive pulmonary disease (COPD), heart disease, or diabetes, are more susceptible to developing shock lung. These conditions can weaken the lungs and make them more vulnerable to injury.
3. Smoking
Smoking is a significant risk factor for many respiratory conditions, including shock lung. The harmful substances in tobacco smoke can damage lung tissue and impair the body’s ability to fight infections.
4. Obesity
Obesity can increase the risk of developing shock lung due to its impact on lung function. Excess weight can restrict lung expansion and lead to breathing difficulties, making individuals more susceptible to respiratory distress.
5. Hospitalization and Mechanical Ventilation
Patients who are hospitalized, especially those requiring mechanical ventilation, are at a higher risk for developing shock lung. The use of ventilators can sometimes lead to ventilator-associated lung injury, which can trigger ARDS.
6. Genetic Factors
Some individuals may have a genetic predisposition that makes them more susceptible to developing shock lung. Research is ongoing to understand the genetic factors that contribute to this condition.
Recognizing these causes and risk factors is essential for healthcare providers and patients alike. By understanding the underlying issues that can lead to shock lung, we can take proactive steps to mitigate risks and improve outcomes. 🌟
Shock Lung Diagnosis
Shock lung, also known as acute respiratory distress syndrome (ARDS), is a serious condition that affects the lungs and can lead to severe respiratory failure. Diagnosing shock lung requires a comprehensive approach, as the symptoms can often mimic other respiratory conditions. Here’s what you need to know about the diagnostic process.
Understanding the Symptoms
The first step in diagnosing shock lung is recognizing its symptoms. Common signs include:
- Severe shortness of breath – Patients may experience difficulty breathing, even at rest.
- Rapid breathing – An increased respiratory rate is often observed.
- Low oxygen levels – This can be measured using a pulse oximeter.
- Chest pain – Discomfort or pain in the chest area may occur.
- Confusion or altered mental state – Due to low oxygen levels, patients may exhibit confusion.
Medical History and Physical Examination
A thorough medical history is crucial in diagnosing shock lung. Healthcare providers will ask about:
- Recent illnesses or infections
- History of lung diseases
- Exposure to toxins or allergens
- Recent surgeries or trauma
During the physical examination, doctors will assess the patient’s breathing patterns, lung sounds, and overall respiratory function. This initial evaluation helps to rule out other conditions that may present similar symptoms.
Diagnostic Tests
To confirm a diagnosis of shock lung, several tests may be conducted:
- Chest X-ray – This imaging test can reveal fluid in the lungs, which is a hallmark of shock lung.
- CT Scan – A more detailed imaging test that provides a clearer view of lung structures.
- Blood Tests – These tests can help identify underlying infections or other contributing factors.
- Arterial Blood Gas (ABG) Test – This test measures oxygen and carbon dioxide levels in the blood, providing insight into lung function.
In some cases, a bronchoscopy may be performed to visualize the airways and collect samples for further analysis. This can help identify infections or other abnormalities.
Shock Lung Treatment Options
Treating shock lung effectively requires a multi-faceted approach, focusing on both the underlying cause and the symptoms. Here are the primary treatment options available:
Oxygen Therapy
One of the first lines of treatment for shock lung is oxygen therapy. This involves administering supplemental oxygen to improve oxygen levels in the blood. Depending on the severity of the condition, this may be done through:
- Nasal cannula – A simple device that delivers oxygen through the nostrils.
- Face mask – Provides a higher concentration of oxygen.
- Mechanical ventilation – In severe cases, patients may require a ventilator to assist with breathing.
Medications
Several medications may be used to treat shock lung, including:
- Antibiotics – If an infection is present, antibiotics will be prescribed.
- Corticosteroids – These can help reduce inflammation in the lungs.
- Diuretics – Used to remove excess fluid from the lungs and improve breathing.
Supportive Care
Supportive care is essential in managing shock lung. This may include:
- Fluid management – Careful monitoring of fluid intake and output to prevent fluid overload.
- Nutritional support – Ensuring patients receive adequate nutrition, often through enteral feeding if they cannot eat normally.
- Physical therapy – Rehabilitation exercises to improve lung function and overall strength.
Addressing Underlying Causes
Identifying and treating the underlying cause of shock lung is crucial for recovery. This may involve:
- Managing infections – Prompt treatment of pneumonia or sepsis.
- Controlling chronic conditions – Such as heart failure or diabetes, which can exacerbate respiratory issues.
In summary, diagnosing and treating shock lung requires a comprehensive approach that addresses both the symptoms and the underlying causes. Early intervention is key to improving outcomes and enhancing recovery. 🌟

Shock Lung Complications
Shock lung, also known as acute respiratory distress syndrome (ARDS), is a serious condition that can arise from various causes, including trauma, pneumonia, and sepsis. Understanding the complications associated with shock lung is crucial for both patients and healthcare providers. Here, we will explore the potential complications that can arise from this condition.
1. Respiratory Failure
One of the most significant complications of shock lung is respiratory failure. This occurs when the lungs are unable to provide adequate oxygen to the bloodstream or remove carbon dioxide effectively. Patients may require mechanical ventilation to support their breathing, which can lead to further complications, such as:
- Ventilator-associated pneumonia: Prolonged mechanical ventilation can increase the risk of infections.
- Barotrauma: High pressures from mechanical ventilation can damage lung tissue.
2. Pulmonary Hypertension
Shock lung can lead to pulmonary hypertension, a condition characterized by increased blood pressure in the pulmonary arteries. This can strain the heart and lead to heart failure if not managed properly. Symptoms may include:
- Shortness of breath
- Fatigue
- Chest pain
3. Multi-Organ Dysfunction
Shock lung is often part of a broader systemic response to injury or infection, which can result in multi-organ dysfunction syndrome (MODS). This condition occurs when multiple organ systems fail, leading to severe complications. Commonly affected organs include:
- Kidneys: Acute kidney injury may occur, requiring dialysis.
- Liver: Liver dysfunction can lead to coagulopathy and metabolic disturbances.
- Heart: Cardiac function may be compromised, leading to arrhythmias or heart failure.
4. Psychological Impact
The experience of shock lung and its treatment can have a profound psychological impact on patients. Many individuals may suffer from post-traumatic stress disorder (PTSD), anxiety, or depression following their recovery. It’s essential for healthcare providers to address these mental health aspects as part of the overall treatment plan.
Preventing Shock Lung
Preventing shock lung is vital for reducing the incidence of this serious condition. While not all cases can be avoided, certain strategies can significantly lower the risk. Here are some effective prevention methods:
1. Early Recognition and Treatment of Underlying Conditions
Identifying and treating conditions that can lead to shock lung, such as pneumonia, sepsis, or trauma, is crucial. Early intervention can prevent the progression to ARDS. Healthcare providers should:
- Monitor patients closely for signs of respiratory distress.
- Administer appropriate antibiotics for infections.
- Manage fluid balance carefully in critically ill patients.
2. Optimizing Ventilation Strategies
For patients requiring mechanical ventilation, using lung-protective ventilation strategies can help minimize lung injury. This includes:
- Using lower tidal volumes to reduce over-distension of alveoli.
- Maintaining appropriate positive end-expiratory pressure (PEEP) to keep alveoli open.
3. Infection Control Measures
Implementing strict infection control measures in healthcare settings can help prevent ventilator-associated pneumonia and other infections that may lead to shock lung. Key practices include:
- Hand hygiene protocols
- Use of sterile techniques during intubation
- Regular cleaning and disinfection of equipment
4. Patient Education
Educating patients and their families about the signs and symptoms of respiratory distress can empower them to seek timely medical attention. Awareness of risk factors, such as smoking and obesity, can also encourage lifestyle changes that promote lung health.
In conclusion, while shock lung presents significant challenges, understanding its complications and implementing preventive measures can greatly improve patient outcomes. By focusing on early intervention, optimizing care strategies, and promoting awareness, we can work towards reducing the incidence of this serious condition. 🌟

Frequently Asked Questions about Shock Lung
What is Shock Lung?
Shock lung, also known as acute respiratory distress syndrome (ARDS), is a serious condition characterized by widespread inflammation in the lungs. This condition can lead to severe breathing difficulties and requires immediate medical attention.
What are the symptoms of Shock Lung?
- Severe shortness of breath
- Rapid breathing
- Low oxygen levels in the blood
- Chest pain
- Fatigue
What causes Shock Lung?
Shock lung syndrome can be triggered by various factors, including:
- Pneumonia
- Sepsis
- Trauma
- Inhalation of harmful substances
- Pancreatitis
How is Shock Lung diagnosed?
Diagnosis of shock lung typically involves a combination of physical examinations, medical history assessments, and imaging tests such as chest X-rays or CT scans to evaluate lung function and identify any underlying issues.
What treatments are available for Shock Lung?
Treatment for shock lung may include:
- Oxygen therapy
- Mechanical ventilation
- Medications to manage inflammation
- Fluid management
Can Shock Lung occur in dogs?
Yes, shock lung in dogs can occur, often as a result of similar underlying conditions that affect humans, such as pneumonia or trauma. If you suspect your pet is experiencing respiratory distress, consult a veterinarian immediately.
What is the prognosis for someone with Shock Lung?
The prognosis for individuals with shock lung varies based on the underlying cause, the severity of the condition, and how quickly treatment is initiated. Early intervention can significantly improve outcomes.
Is Shock Lung associated with ARDS stages?
Shock lung is seen in which stage of ARDS can depend on the severity of the lung injury. ARDS is classified into mild, moderate, and severe stages, with shock lung typically being associated with moderate to severe cases.
Where can I find more information about Shock Lung?
For more detailed information, consider consulting medical literature or speaking with healthcare professionals who specialize in respiratory conditions.




