What Is Sweet Syndrome?
Sweet Syndrome, also known as acute febrile neutrophilic dermatosis, is a rare skin condition characterized by the sudden onset of fever and painful skin lesions. First described in 1964 by Dr. Robert Sweet, this syndrome primarily affects adults, although it can occur in children as well. The exact cause of Sweet Syndrome remains unclear, but it is often associated with underlying conditions such as infections, malignancies, or autoimmune diseases.
Sweet Syndrome is classified as a type of neutrophilic dermatosis, which means it involves an abnormal accumulation of neutrophils (a type of white blood cell) in the skin. This accumulation leads to inflammation and the characteristic symptoms of the syndrome. Understanding Sweet Syndrome is crucial for timely diagnosis and effective treatment.
Causes of Sweet Syndrome
The precise cause of Sweet Syndrome is still a topic of research, but several factors have been identified that may trigger its onset:
- Infections: Certain infections, particularly upper respiratory infections, can precede the development of Sweet Syndrome.
- Malignancies: There is a notable association between Sweet Syndrome and various cancers, especially hematological malignancies like leukemia.
- Autoimmune Diseases: Conditions such as inflammatory bowel disease and rheumatoid arthritis have been linked to Sweet Syndrome.
- Medications: Some medications, particularly those that stimulate the immune system, may trigger the syndrome.
Sweet Syndrome Symptoms
The symptoms of Sweet Syndrome can vary from person to person, but they typically include:
Skin Lesions
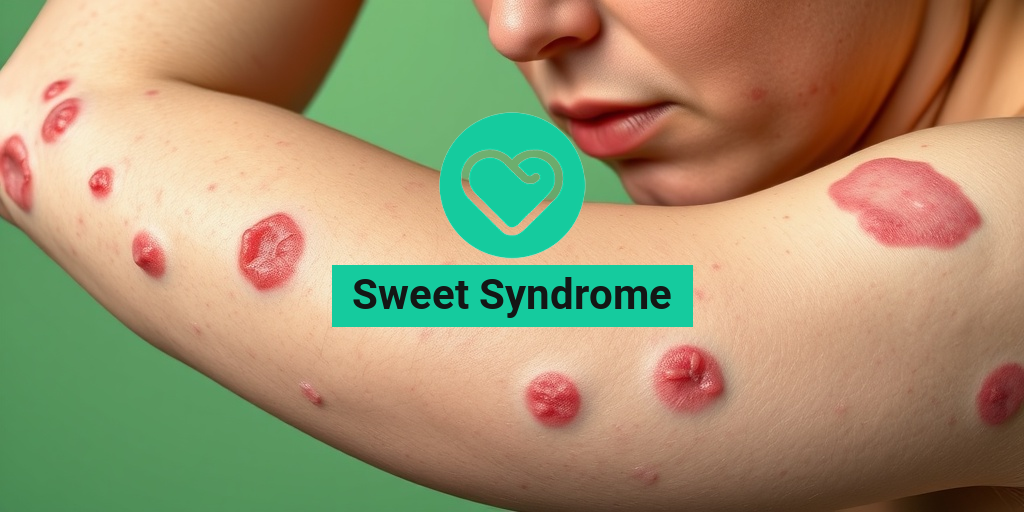
The most prominent feature of Sweet Syndrome is the appearance of skin lesions. These lesions are usually:
- Red or purple: The lesions often have a bright red or purplish hue.
- Raised: They are typically raised above the skin surface.
- Painful: Many individuals report significant pain or tenderness in the affected areas.
- Location: Lesions commonly appear on the arms, face, neck, and trunk.
Systemic Symptoms
In addition to skin lesions, Sweet Syndrome can present with systemic symptoms, including:
- Fever: A high fever is often one of the first symptoms to appear.
- Malaise: General feelings of discomfort or unease are common.
- Joint Pain: Some individuals may experience arthralgia (joint pain).
Diagnosis and Treatment
Diagnosing Sweet Syndrome typically involves a combination of clinical evaluation and laboratory tests. A dermatologist may perform a skin biopsy to confirm the presence of neutrophilic infiltration, which is a hallmark of the condition.
Treatment for Sweet Syndrome often includes:
- Corticosteroids: These are the mainstay of treatment and can help reduce inflammation and alleviate symptoms.
- Immunosuppressive Agents: In more severe cases, medications that suppress the immune system may be necessary.
- Treating Underlying Conditions: If Sweet Syndrome is associated with an underlying disease, addressing that condition is crucial for effective management.
For those seeking more information on Sweet Syndrome and its management, Yesil Health AI offers a wealth of evidence-based health answers and resources.
In conclusion, Sweet Syndrome is a complex condition that requires careful diagnosis and management. If you or someone you know is experiencing symptoms consistent with Sweet Syndrome, it is essential to consult a healthcare professional for appropriate evaluation and treatment. 🌟

Sweet Syndrome Causes
Sweet Syndrome, also known as acute febrile neutrophilic dermatosis, is a rare skin condition characterized by painful, red, and swollen lesions. Understanding the causes of Sweet Syndrome is crucial for effective diagnosis and treatment. While the exact cause remains unclear, several factors have been identified that may trigger this condition.
Underlying Medical Conditions
Sweet Syndrome is often associated with various underlying medical conditions. Some of the most common include:
- Hematological Disorders: Conditions like leukemia and myelodysplastic syndromes are frequently linked to Sweet Syndrome. These disorders can lead to an abnormal immune response, resulting in skin lesions.
- Infections: Certain infections, particularly those caused by bacteria or viruses, can trigger Sweet Syndrome. For instance, Streptococcus infections have been noted as potential culprits.
- Autoimmune Diseases: Diseases such as Crohn’s disease and ulcerative colitis may also be associated with Sweet Syndrome, suggesting a connection between immune system dysfunction and skin manifestations.
Medications
Some medications have been reported to induce Sweet Syndrome. These include:
- Granulocyte-colony stimulating factor (G-CSF): Used to stimulate the production of white blood cells, G-CSF has been linked to the onset of Sweet Syndrome in some patients.
- Antibiotics: Certain antibiotics, particularly those that affect the immune system, may trigger the condition.
Genetic Factors
While research is still ongoing, there may be a genetic predisposition to Sweet Syndrome. Individuals with a family history of autoimmune diseases or skin conditions may be at a higher risk. Genetic factors can influence how the immune system responds to various triggers, potentially leading to the development of Sweet Syndrome.
Sweet Syndrome Risk Factors
Identifying the risk factors for Sweet Syndrome can help in early detection and management of the condition. While anyone can develop Sweet Syndrome, certain groups may be more susceptible.
Demographic Factors
Sweet Syndrome is more commonly diagnosed in women than in men, particularly those in their 30s to 60s. This demographic trend suggests that hormonal factors may play a role in the development of the condition.
Pre-existing Health Conditions
Individuals with certain health conditions are at a higher risk for developing Sweet Syndrome. These include:
- Blood Disorders: As mentioned earlier, those with blood-related conditions, especially leukemias, are at increased risk.
- Autoimmune Diseases: A history of autoimmune disorders can heighten the likelihood of developing Sweet Syndrome.
Environmental Triggers
Environmental factors may also contribute to the onset of Sweet Syndrome. These can include:
- Infections: Exposure to certain infections, particularly bacterial infections, can act as a trigger.
- Stress: Physical or emotional stress may exacerbate underlying conditions, potentially leading to the development of Sweet Syndrome.
Age and Gender
As previously noted, age and gender are significant risk factors. Women, particularly those in their reproductive years, are more likely to develop Sweet Syndrome. This may be linked to hormonal changes that occur during this time.
In summary, while the exact causes of Sweet Syndrome remain elusive, understanding the potential triggers and risk factors can aid in early diagnosis and treatment. If you suspect you or someone you know may be experiencing symptoms of Sweet Syndrome, it’s essential to consult a healthcare professional for a thorough evaluation and appropriate management. 🩺

Sweet Syndrome Diagnosis
Diagnosing Sweet Syndrome can be a complex process, as it often mimics other skin conditions and systemic diseases. This rare inflammatory disorder is characterized by the sudden onset of painful skin lesions, fever, and other systemic symptoms. To accurately diagnose Sweet Syndrome, healthcare providers typically follow a series of steps.
Clinical Evaluation
The first step in diagnosing Sweet Syndrome involves a thorough clinical evaluation. Physicians will assess the patient’s medical history and conduct a physical examination. Key symptoms to look for include:
- Fever: Often present at the onset of the condition.
- Painful skin lesions: These can appear as red, swollen bumps or plaques, commonly found on the arms, face, and neck.
- Other systemic symptoms: Such as malaise, fatigue, and joint pain.
Skin Biopsy
A definitive diagnosis of Sweet Syndrome often requires a skin biopsy. During this procedure, a small sample of the affected skin is removed and examined under a microscope. Pathologists look for specific histological features, such as:
- Neutrophilic infiltration: A hallmark of Sweet Syndrome, where neutrophils accumulate in the upper dermis.
- Absence of vasculitis: Differentiating it from other conditions that may present similarly.
Laboratory Tests
In addition to a skin biopsy, laboratory tests may be conducted to rule out other conditions. These tests can include:
- Blood tests: To check for elevated white blood cell counts and inflammatory markers.
- Imaging studies: In some cases, imaging may be necessary to assess for underlying systemic involvement.
It’s important to note that Sweet Syndrome can be associated with underlying conditions, such as malignancies or autoimmune diseases. Therefore, a comprehensive evaluation is crucial for effective diagnosis and management. 🩺
Sweet Syndrome Treatment Options
Treating Sweet Syndrome focuses on alleviating symptoms and addressing any underlying conditions. The treatment plan may vary depending on the severity of the symptoms and the patient’s overall health. Here are some common treatment options:
Medications
Medications are often the first line of treatment for Sweet Syndrome. Commonly prescribed options include:
- Systemic corticosteroids: These are the most effective treatment for reducing inflammation and controlling symptoms. Prednisone is frequently used and can lead to rapid improvement.
- Non-steroidal anti-inflammatory drugs (NSAIDs): These can help manage pain and inflammation.
- Immunosuppressive agents: In cases where corticosteroids are ineffective or if the condition is recurrent, medications like azathioprine or methotrexate may be considered.
Topical Treatments
For mild cases of Sweet Syndrome, topical treatments may be sufficient. These can include:
- Topical corticosteroids: Applied directly to the affected areas to reduce inflammation and discomfort.
- Moisturizers: Keeping the skin hydrated can help alleviate dryness and irritation associated with the rash.
Addressing Underlying Conditions
If Sweet Syndrome is associated with an underlying condition, such as a malignancy or autoimmune disorder, treating that condition is crucial. This may involve:
- Cancer treatment: If a malignancy is identified, appropriate oncological interventions will be necessary.
- Management of autoimmune diseases: Tailoring treatment plans for conditions like rheumatoid arthritis or inflammatory bowel disease can help reduce the incidence of Sweet Syndrome flare-ups.
In conclusion, while Sweet Syndrome can be challenging to diagnose and treat, a combination of medications, topical treatments, and addressing any underlying conditions can lead to effective management. If you suspect you have Sweet Syndrome, it’s essential to consult a healthcare professional for a comprehensive evaluation and personalized treatment plan. 🌟
Sweet Syndrome Management
Managing Sweet Syndrome effectively requires a comprehensive approach that includes accurate diagnosis, treatment, and ongoing care. This rare condition, characterized by fever, painful skin lesions, and a variety of systemic symptoms, can be challenging to navigate. Here’s a closer look at how to manage this condition effectively.
Diagnosis and Initial Assessment
The first step in managing Sweet Syndrome is obtaining a correct diagnosis. This typically involves:
- Clinical Evaluation: A thorough examination by a healthcare professional is essential. They will assess the characteristic symptoms, including the distinctive rash.
- Skin Biopsy: A biopsy of the affected skin can confirm the diagnosis by revealing the presence of neutrophilic infiltrates.
- Blood Tests: These tests can help rule out other conditions and assess inflammatory markers.
Treatment Options
Once diagnosed, treatment can begin. The primary goal is to alleviate symptoms and address the underlying causes. Here are some common treatment options:
- Corticosteroids: These are the first-line treatment for Sweet Syndrome. Oral corticosteroids like prednisone can significantly reduce inflammation and improve symptoms.
- Immunosuppressive Agents: In cases where corticosteroids are ineffective or if the syndrome is recurrent, medications such as azathioprine or mycophenolate mofetil may be prescribed.
- Topical Treatments: For localized skin lesions, topical corticosteroids can provide relief.
- Management of Underlying Conditions: If Sweet Syndrome is associated with another disease (like cancer or autoimmune disorders), treating that condition is crucial.
Supportive Care
In addition to medical treatments, supportive care plays a vital role in managing Sweet Syndrome:
- Pain Management: Over-the-counter pain relievers can help alleviate discomfort associated with skin lesions.
- Skin Care: Keeping the skin moisturized and protected can prevent further irritation and promote healing.
- Regular Follow-ups: Ongoing monitoring with a healthcare provider is essential to adjust treatment plans as needed.
Sweet Syndrome Prognosis
The prognosis for individuals with Sweet Syndrome can vary significantly based on several factors, including the underlying cause and the timeliness of treatment. Understanding the potential outcomes can help patients and their families prepare for the journey ahead.
Factors Influencing Prognosis
Several factors can influence the prognosis of Sweet Syndrome:
- Underlying Conditions: If Sweet Syndrome is secondary to another disease, such as malignancy or autoimmune disorders, the prognosis may depend on the management of that condition.
- Response to Treatment: Most patients respond well to corticosteroids, leading to a significant reduction in symptoms. However, some may experience recurrences.
- Age and Overall Health: Younger patients and those in good overall health tend to have a better prognosis.
Long-term Outlook
For many patients, Sweet Syndrome can be a self-limiting condition, especially when effectively treated. However, some individuals may experience:
- Recurrences: While treatment can lead to remission, some patients may have recurrent episodes of Sweet Syndrome.
- Chronic Symptoms: In rare cases, patients may develop chronic symptoms that require ongoing management.
Overall, with appropriate treatment and management strategies, the prognosis for Sweet Syndrome is generally favorable. Patients are encouraged to maintain open communication with their healthcare providers to ensure the best possible outcomes. 🌟

Frequently Asked Questions about Sweet Syndrome
What is Sweet Syndrome?
Sweet Syndrome, also known as acute febrile neutrophilic dermatosis, is a rare skin condition characterized by painful, red, and swollen lesions. It often appears suddenly and can be associated with fever and other systemic symptoms.
What are the common symptoms of Sweet Syndrome?
- Rash: The most prominent symptom is a rash that typically consists of raised, red bumps or plaques.
- Pain: The lesions can be painful and tender to the touch.
- Fever: Many patients experience a fever along with the skin symptoms.
- Other Symptoms: Fatigue, malaise, and joint pain may also occur.
What causes Sweet Syndrome?
The exact cause of Sweet Syndrome is not fully understood. However, it can be triggered by various factors, including:
- Infections
- Medications
- Underlying diseases, such as hematological malignancies
- Pregnancy
How is Sweet Syndrome diagnosed?
Diagnosis typically involves a combination of clinical evaluation and skin biopsy. The biopsy helps to confirm the presence of neutrophilic infiltration, which is characteristic of Sweet Syndrome.
What are the treatment options for Sweet Syndrome?
Treatment for Sweet Syndrome often includes:
- Corticosteroids: These are the first-line treatment and can help reduce inflammation and symptoms.
- Other Medications: In some cases, immunosuppressive agents or other medications may be used.
- Management of Underlying Conditions: Addressing any underlying triggers is crucial for effective treatment.
Are there any pictures of Sweet Syndrome rash available?
Yes, there are many Sweet Syndrome rash pictures available online that can help you identify the condition. However, it is always best to consult a healthcare professional for an accurate diagnosis.
What is the ICD-10 code for Sweet Syndrome?
The ICD-10 code for Sweet Syndrome is L98.0. This code is used for billing and documentation purposes in medical settings.
Can Sweet Syndrome be prevented?
While there is no guaranteed way to prevent Sweet Syndrome, managing underlying health conditions and avoiding known triggers may help reduce the risk of flare-ups.
Where can I find more information about Sweet Syndrome?
For more detailed information, you can visit reputable medical websites or consult with a dermatologist who specializes in skin disorders.